Breast Reconstruction
 The decision to have breast reconstruction is an important and personal one and requires a thorough understanding of all options available. While breast reconstruction is not the choice for everyone, many women who have undergone reconstruction experience significant improvement in their emotional well-being and physical appearance. The American College of Surgeons Commission on Cancer (CoC) requires that all women who are considering mastectomy be offered a consultation with a plastic surgeon to discuss reconstruction options prior to surgery.
The decision to have breast reconstruction is an important and personal one and requires a thorough understanding of all options available. While breast reconstruction is not the choice for everyone, many women who have undergone reconstruction experience significant improvement in their emotional well-being and physical appearance. The American College of Surgeons Commission on Cancer (CoC) requires that all women who are considering mastectomy be offered a consultation with a plastic surgeon to discuss reconstruction options prior to surgery.
The office of our experienced plastic surgeon, Dr. Max Lehfeldt, is dedicated to achieving your goals and exceeding your expectations. We have cared for thousands of breast cancer survivors! Breast cancer and reconstruction can be a very daunting and challenging process and we are here to help you navigate through these difficult decisions. We look forward to taking care of you!
Below you will find Dr. Lehfeldt’s comprehensive review of breast reconstruction options. These should assist you with your decisions but should not replace a formal consultation with Dr. Max Lehfeldt. His goal is to help you determine the ideal reconstructive choice that best fits your unique needs and circumstances.
- Timing of Reconstruction
- Types of Reconstruction
- Single-Stage Direct to Implant Reconstruction
- Tissue Expanders
- Latissimus Flap with Implant Reconstruction
- Delayed Immediate Reconstruction
- Oncoplastic Reconstruction
- Nipple Areola Reconstruction
Timing of Reconstruction
The breast reconstruction process may begin:
- Immediately: At the time of your mastectomy. Most patients today experience maximum aesthetic and psychological benefits with an immediate reconstruction.
- Delayed: Weeks to years after your mastectomy.
- Delayed/Immediate: Where a temporary tissue expander or implant is placed at the time of mastectomy to be later replaced with your own tissue (“flap”). This approach is often used for patients who are at high risk for post-mastectomy radiation therapy. This two-step approach is used to avoid radiating the flap tissue and still allows for minimum scarring and maximum preservation of chest wall and breast skin.
Types of Reconstruction
There are six commonly performed types of breast reconstruction:
- A direct-to-implant (single-stage) reconstruction where no tissue expander is required.
- A tissue expander followed by a second surgery for removal of the tissue expander and placement of breast implant (silicone gel or saline).
- Flap reconstruction – a breast may be reconstructed from your own tissues – abdomen, upper back, or inner thighs.
The tissues may be left attached to the blood supply and rotated to the breast area; this is known as a pedicle flap. Or tissues may be removed completely, reattached at the breast area under a microscope; this is known as a free flap.
Common flap surgeries include:
- Latissimus Dorsi (upper back skin and muscle)
- Latissimus flap with implant reconstruction – a combination of both a flap and tissue expander or implant.
- A delayed-immediate reconstruction where a temporary tissue expander or implant is used to maintain the chest wall/breast skin envelope. The patient will then receive post-mastectomy radiation, then return for surgery to remove the tissue expander and replace it with flap tissue.
- Oncoplastic reconstruction is ideal for lumpectomy patients and breast conservation surgery. Using modified breast reduction incision patterns and local breast tissue repositioning, we are able to maintain maximum breast aesthetics.
Single-Stage Direct to Implant Reconstruction
There are circumstances where breast reconstruction can be performed without the need for a tissue expander. Women who are candidates for nipple-preserving mastectomy are often good candidates for direct-to-implant reconstruction.
This technique has the added convenience of avoiding office visits for expansion and the additional step of removing and replacing the expander. The duration of surgery is similar to that for tissue expander reconstruction (one to three hours). Direct-to-implant reconstruction requires one to two nights of hospitalization and about two to three weeks of recovery. This type of reconstruction is best suited for women with very healthy mastectomy skin flaps who have sufficient skin to accommodate an implant at the time of mastectomy. Direct to implant reconstruction is ideal for nipple-preserving mastectomy. It is also ideal for patients with existing implants. However, there are potentially slightly higher risks for healing problems with this approach due to the added “pressure” that may be placed on the mastectomy skin by the implant. The need for additional surgery to “fine tune” the results is approximately 50%.
Tissue Expanders
This procedure can be performed immediately (at the time of mastectomy) or delayed (weeks to years after the mastectomy).
The aesthetic goal of a tissue expander or implant reconstruction is to “look good in a bra.” These devices do a good job of recreating a breast mound and filling a bra. Tissue expanders and breast implants are a good option for smaller breasted women who do not have a lot of excess tissue for flap reconstructions. Expanders/implants do not exactly replicate large hanging breasts and, therefore, are not the best option for patients with larger, droopy breasts or for patients who desire a more “natural” look. Expander/implant reconstructions are ideally suited for patients who are having both breasts reconstructed but also can be done for unilateral reconstruction as well. Expander/implant reconstructions are also best suited for smaller breasted women. It is often easier to achieve breast symmetry when reconstructing both breasts using this technique.
A tissue expander is an elastic, silicone, rubber device placed under the breast skin and pectoralis muscle to support and maintain the position of the expander. A single side reconstruction takes about an hour to two hours and bilateral reconstructions may take up to three hours. The hospital stay is usually one to two nights. Recovery is around two to three weeks.
After the Placement of Your Expander
Starting about three weeks after placement of the expander, Dr. Lehfeldt will start filling the expander with sterile saline via a small needle inserted through the skin (breast skin is usually numb following mastectomy). You may experience feelings of pressure or discomfort after each filling of the expander (similar to the aches and pains following a vigorous workout). These feelings last only a few hours and are easily managed with ibuprofen. Dr. Lehfeldt’s use of soft tissue supports in tissue expander breast reconstruction allows him to fill the expander a minimum of 50% at the time of surgery/reconstruction and sometimes more. This expansion at the time of surgery often improves the breast shape right away and further reduces the number of visits required to expand and fill the tissue expanders. Often patients can be fully expanded in less than 2-3 visits! This shortened time interval has great psychological benefits for patients.
Gradually, the tissue over the tissue expander device expands, stretches, and creates a pocket for the breast implant. The permanent breast implants are usually inserted 3 months after the expander was placed. Dr. Lehfeldt will evaluate your shape and desired breast volume to help determine the appropriate implant. The beauty of an expander/implant reconstruction is that you, the patient, can actively participate in the process and have the opportunity to decide the size of breast you want!
*Use of Alloderm or Strattice in breast surgery (cosmetic or reconstructive) is not approved by the FDA. Use of these materials in breast surgery is considered an off-label use.
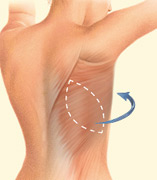
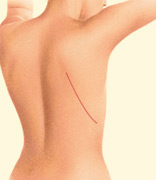
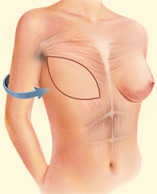
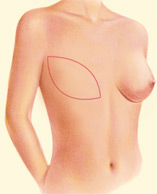
Latissimus Flap with Implant Reconstruction
During latissimus dorsi flap breast reconstruction, muscle and skin tissue are removed from an area of the back and used to help reconstruct the breast. Latissimus dorsi flaps typically have less fat and are usually thinner than TRAM or DIEP flaps. To enhance the volume and shape of the reconstructed breast, an implant is commonly placed under the flap.
This technique is often used for patients that are thin and do not have other suitable tissue donor sites for reconstruction. The latissimus dorsi is also used for patients that have had previous chest wall or breast radiation that wish to use breast implants. The latissimus dorsi muscle is used to “wrap” around the implant and to protect it from the radiated tissue. This reduces the rate of scar tissue formation that can form around implants (encapsulation). The latissimus dorsi flap procedure typically takes two to four hours of surgery. The hospital stay is typically two to three days. Most patients resume normal activities about three weeks after surgery. There may be some weakness in the shoulder and back area as a result of the latissimus muscle repositioning. There will also be a scar on your back which usually can be hidden in the bra line. There are “short-scar” or minimally invasive latissimus harvest techniques (with the use of an endoscope) that can dramatically minimize the back scar. Latissimus flaps often require drains for up to two to three weeks.
Delayed Immediate Reconstruction
This is a “hybrid” reconstruction technique that uses an expander or implant at the time of mastectomy followed by a second operation with a flap procedure.
This approach is used for patients who are at high risk for post-mastectomy radiation. Radiation creates additional scar tissue that can damage the flap tissue. In order to minimize the damaging effects of the radiation and to maximize the preservation of breast skin, a temporary tissue expander or implant is placed at the time of the mastectomy to maintain the breast skin envelope. The expander or implant maintains the skin shape during radiation treatments. Following completion of the radiation therapy, the expander or implant is removed and replaced with a flap. This two-step technique allows for maximum preservation of breast skin while minimizing scarring and minimizing scar tissue formation within the flap from exposure to radiation.
More and more patients are requiring post-mastectomy radiation. Although radiation is often a critical component to successful rates of cure, it has a significant impact on breast reconstruction. Radiation may lead to high rates of scar tissue formation around breast implants (>50%). Radiated implants may become firm, tight, and even uncomfortable. This is known as capsular contracture. Flap reconstructions exposed to radiation can also develop areas of scar tissue and firmness (fat necrosis). Radiation does not preclude reconstruction, but it often requires additional surgical procedures (delayed/immediate reconstruction, etc.) to correct or prevent radiation-induced scar tissue. Radiated tissue is also associated with higher rates of wound healing problems and other complications.
Oncoplastic Reconstruction
In cases where mastectomy is not required, a lumpectomy can be performed. When the tissue to be removed with the lumpectomy is significant in size or is isolated to a very conspicuous location, a contour deformity may result. In order to minimize the deforming effects of lumpectomy, oncoplastic manipulation of the tissue can be performed. Oncoplastic reconstructions utilize cancer-free breast tissue to fill-in and conceal lumpectomy defects. This is often done via breast lift or reduction incisions. Operating room time may be an hour to four hours. A hospital stay is usually not required, and recovery is usually one to two weeks. Post-lumpectomy radiation will be required and may further alter the shape and size of the breast.
In one-sided or unilateral breast reconstruction, it may be difficult to exactly match the remaining breast. This is particularly the case when a patient has large breasts or if the breasts have sagged with age or from breast-feeding. In order to help improve symmetry between your natural and reconstructed breasts, a breast lift, a breast reduction, or a breast augmentation may be required. These procedures are part of your reconstruction and will be covered by your insurance. Modifications to the normal breasts are often performed near the completion of the reconstructive process on an outpatient surgical basis.
Nipple Areola Reconstruction
During many mastectomies, the nipple and areola are removed (skin-sparing mastectomy). However, there are circumstances that may allow you to preserve the nipple (nipple-sparing mastectomy). You can discuss this option with your oncologic surgeon.
However, if the nipple and areola are removed, a very life-like reconstruction can be created. Creation of the nipple is often an outpatient or office procedure that uses skin from the breast in combination with a skin graft taken from another part of the body (inner thigh or abdomen). The color can then be added with a tattoo that can conceal the mastectomy scar. The nipple is often the final step in the reconstructive process.
Please call 888.96.DR.MAX (888.963.7629) or email to make your appointment today and to see if breast reconstruction with Dr. Lehfeldt is right for you!